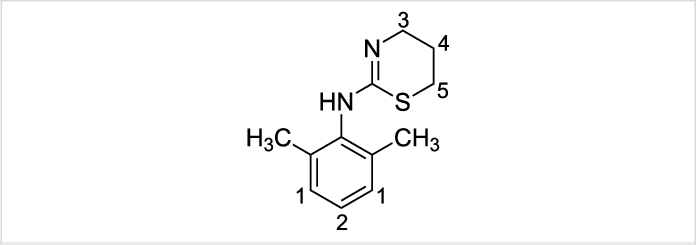
Recent statistics pertaining to drug-related deaths are daunting because of the use of fentanyl. Langer and Chen (2023) report that about 110,000 people in the U.S. died of drug overdoses last year, more than twice as many as five years ago, and in nearly every case, the victims had fentanyl in their blood.
Their article concentrates on the situation in San Francisco. An average of two people currently die from overdoses here every day, a rate 40% higher than a year ago. In the pandemic years of 2020 and 2021, drugs caused more deaths than COVID-19, homicides and traffic accidents combined.
And now the situation is getting even worse. Not so long ago, fentanyl was added to heroin to increase potency and to increase profits for the manufacturer and seller. Now, we are finding that fentanyl is the “primary” drug of choice, and it is being contaminated with xylazine, AKA “tranq” . According to the Director of the US Drug Enforcement Administration, “Xylazine is making the deadliest drug threat our country has ever faced, fentanyl, even deadlier,” said Administrator Milgram. “DEA has seized xylazine and fentanyl mixtures in 48 of 50 States. The DEA Laboratory System is reporting that in 2022 approximately 23% of fentanyl powder and 7% of fentanyl pills seized by the DEA contained xylazine.” ( https://www.dea.gov/alert/dea-reports-widespread-threat-fentanyl-mixed-xylazine )
The report goes further: “According to the CDC, 107,735 Americans died between August 2021 and August 2022 from drug poisonings, with 66 percent of those deaths involving synthetic opioids like fentanyl. The Sinaloa Cartel and Jalisco Cartel in Mexico, using chemicals largely sourced from China, are primarily responsible for the vast majority of the fentanyl that is being trafficked in communities across the United States.”
Laboratory studies with mice show a synergistic effect between fentanyl and xylazine. For example, Smith et. al. (2023) exposed male and female mice to xylazine alone, xylazine + 56 mg/kg fentanyl, fentanyl, and fentanyl + 100 mg/kg xylazine to determine LD20, LD50, and LD80, i.e. the dose required to kill 20%, 50% and 80% of the test animals, respectively. The following table of LD50 results is adapted from their Table I:
| Xylazine alone | Xylazine + 56 mg/kg Fentanyl | Fentanyl alone | Fentanyl + 100 mg/kg Xylazine | |
| Males and females combined | 157.2 | 32.0 | 131.3 | 1.27 |
| Males only | 156.1 | 21.8 | 122.4 | 1.09 |
| Females only | 176.7 | 80.6 | 195.8 | 6.87 |
While xylazine is not approved for human use, it is approved for veterinary use by the US Food and Drug Administration. It is a non-narcotic compound utilized for sedation, pain relief, and muscle relaxation in veterinary medicine.
Xylazine produces a sedative effect by triggering a rapid decrease in the release of norepinephrine and dopamine in the central nervous system (Pergolizzi, et. al., 2023).
Approval was not granted for human use as an antihypertensive due to profound hypotension and excessive central nervous system depression. Xylazine is frequently used with ketamine as an anesthetic agent for experimental studies involving dogs, cats, horses, rabbits, and rats. (Papudesi, et. al., 2023.)
To further quote Papudesi, et. al., (2023):
“Xylazine emerged as a popular illegal substance among those who inject drugs in Puerto Rico in the early 2000s. Currently, there is limited information about the unlawful consumption, geographic prevalence, and immediate or long-term effects of xylazine on humans. Recently, xylazine misuse has surged in the northeastern United States, spreading across many states, as evidenced by the rising number of samples testing positive for the drug.
In Philadelphia, xylazine is popularly referred to as “tranq”; when xylazine is mixed with more prevalent illegal opioids like heroin or fentanyl, the mixture is called “tranq dope.” Xylazine is frequently combined with synthetic opioids, primarily fentanyl, in the unregulated market. Additionally, xylazine has been found alongside cocaine and methamphetamine and, more recently, mixed with oxycodone and alprazolam. Xylazine was reportedly diverted from the veterinary market to the recreational drug market in Puerto Rico.
Xylazine has spread rapidly due to several factors, including cost-cutting, an increase in its addictive properties, and its ability to extend the duration of the opioid with which it is combined. Xylazine poses a challenge to the United States healthcare system and those who use it knowingly or unknowingly due to its benefits to the illegal drug industry, a lack of information, and the absence of an approved antidote.
Xylazine toxicity is characterized by CNS depression. Symptoms may include the following:
- a “high” feeling, sedation
- dry mouth
- dysarthria (difficulty in articulating words due to disease of the central nervous system)
- hyporeflexia (underactivity of bodily reflexes)
- disorientation
- dysmetria (impaired ability to estimate distance in muscular action)
- miosis (excessive smallness or contraction of the pupil of the eye)
- hypotension
- bradycardia (relatively slow heart action)
- hypothermia ( subnormal temperature of the body), and
- hyperglycemia (excess of sugar in the blood).
N.B. Definitions are from the medical division of the online Merriam-Webster dictionary, merriam-webster.com .
When combined with other CNS depressants such as opioids, benzodiazepines, or alcohol, xylazine overdose causes severe CNS depression with signs and symptoms of obtundation, coma, muscle relaxation, hypotension or hypertension, respiratory depression, areflexia, asthenia or apnea, cardiac arrhythmias or cardiac arrest.
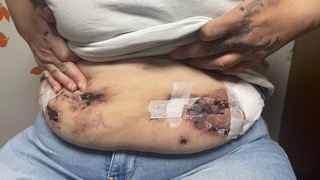
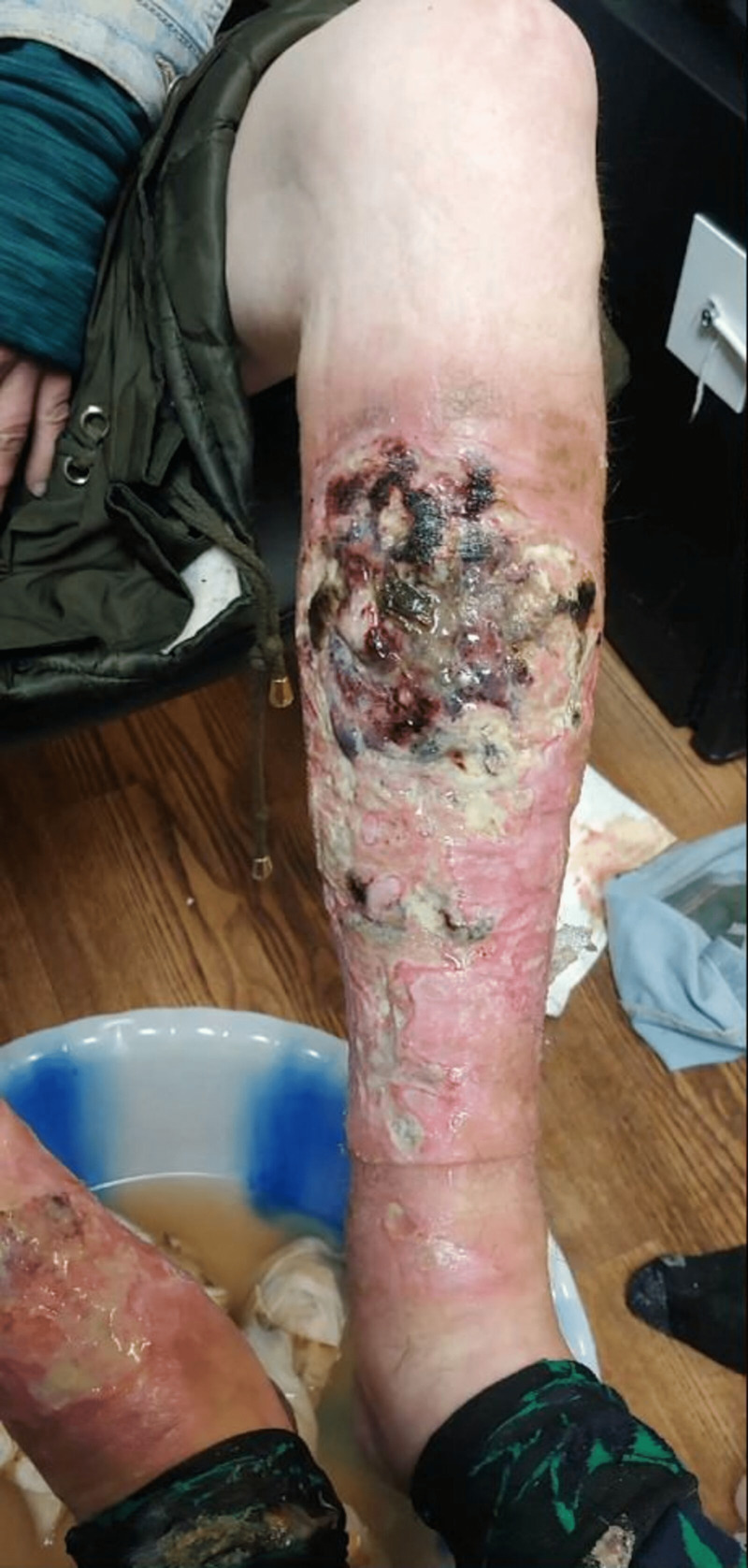
The xylazine high may last up to 6 hours, and users often feel driven to look for their next dosage while still high. This makes abstinence difficult. The lack of effective withdrawal treatment makes abstinence difficult, as standard medication-assisted therapies for opioid use disorder do not mitigate xylazine withdrawal symptoms. The chronic use of heroin and fentanyl mixed with xylazine can lead to deep skin ulcers, abscesses, and infections. These xylazine-associated wounds (like the ones shown below) may increase the risk of bacteremia, endocarditis, sepsis, limb amputation, and death. Any patient with a nonhealing ulcer, regardless of the use of injection as the route of administration, should be assessed for xylazine use.”
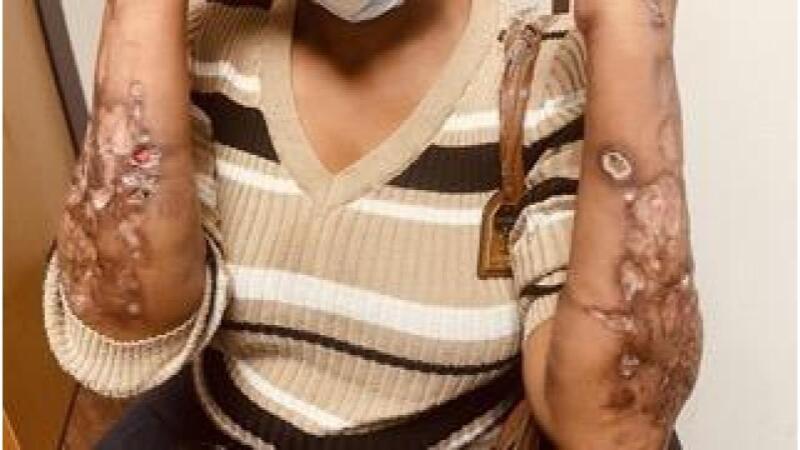
https://www.dea.gov/alert/dea-reports-widespread-threat-fentanyl-mixed-xylazine
Langer, M-A, L.; Chen, M.K. (2023). Fentanyl is destroying San Franciso’s soul. https://www.nzz.ch/english/fentanyl-is-destroying-san-franciscos-soul-ld.1749900
Papudesi BN; Malayala SV; Regina AC. (2023). Xylazine Toxicity. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan–.PMID: 37603662
Pergolizzi J Jr; LeQuang JAK; Magnusson P; Miller TL; Breve F; Varrassi G. (2023). The New Stealth Drug on the Street: A Narrative Review of Xylazine as a Street Drug. Cureus. 2023 Jun 26;15(6):e40983. doi: 10.7759/cureus.40983. eCollection 2023 Jun.PMID: 37503500
Smith MA; Biancorosso SL; Camp JD; Hailu SH; Johansen AN; Morris MH; Carlson HN. (2023). Tranq-dope overdose and mortality: lethality induced by fentanyl and xylazine. Frontiers in Pharmology 2023 Oct 26; 14:1280289. doi: 10.3389/fphar.2023.1280289.
