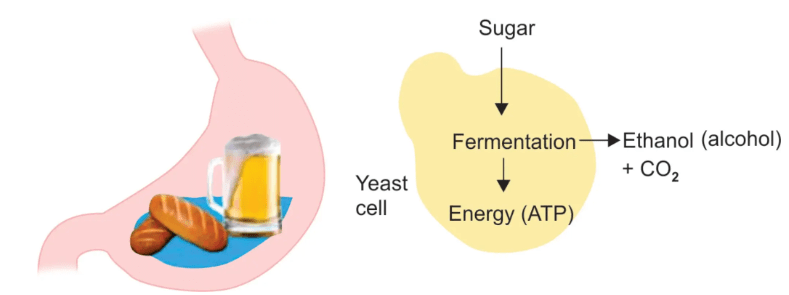
(Infographic from https://vajiramandravi.com/current-affairs/auto-brewery-syndrome/ )
It’s a rare but debilitating condition, in which fungi and/or bacteria capable of synthesizing ethanol get established in the gut. The ethanol these organisms produce is absorbed into the body, and then the person acts intoxicated. In fact, (s)he is intoxicated, showing the following behaviors ( https://my.clevelandclinic.org/health/diseases/auto-brewery-syndrome ):
- Brain fog
- Clumsiness
- Delayed reaction time
- Drowsiness
- Impaired judgment
- Memory issues
- Reduced inhibitions
Case histories often describe the symptoms of auto-brewery syndrome starting after a patient has been prescribed an antibiotic to treat another condition.
For example, Malik, et. al. (2019) describe a case involving a “previously active, healthy, 46-year-old man (height, 6 feet 2 inches; weight, 230 lbs; body mass index, 30 kg/m2) with no significant medical or psychiatric history sought our help for the confirmation and treatment of ABS (Auto-Brewery Disease).” He complained of having had memory loss, mental changes, and episodes of depression for over 6 years starting in January of 2011, following treatment with an antibiotic (cephalexin) for a complicated traumatic thumb injury. While undergoing treatment, his blood alcohol concentration varied from 50 to 400 mg/dL (.05 to 0.4%)(!). Tests revealed the presence of Saccharomyces cerevisiae (brewer’s yeast), S. boulardii, Candida albicans and C. parapsilosis in his intestinal flora. Treatment was successful after administration of probiotic (single-strain Lactobacillus acidophilus with 3 billion colony-forming units per capsule) to competitively inhibit fungi and help to normalise his gut flora. This treatment with a single strain was followed with a multistrain administration.
In many cases, patients show significant inebriation following the consumption of a high carbohydrate diet.
Painter, et. al. (2023) list several species of fungi and bacteria capable of synthesizing ethanol which are the culprits in generating this syndrome:
- Fungi
- Fermenting yeasts such as Saccharomyces cerevisiae, S boulardii;
- Various strains of Candida, including C glabrata, C albicans, C kefyr, and C parapsilosis;
- Bacteria
- Klebsiella pneumonia;
- Enterococcus faecium;
- E. faecalis; and
- Citrobacter freundii.
Treatment involves the following:
- Immediate care for acute alcohol poisoning;
- Drug therapy: To identify the yeast or bacteria responsible for generating endogenous ethanol. Most patients require treatment with azoles and/or polyenes;
- Diet therapy: Since severe episodes of intoxication are induced following the consumption of a high carbohydrate diet, An essential treatment of auto-brewery syndrome is diet modification requiring high protein and low carbohydrates until symptoms subside’. Sugar is fermented into alcohol, and a diet that eliminates simple and complex sugars will decrease the alcohol fermented from the gastrointestinal and genitourinary tract;
- Supplements: “Multistrain probiotic supplements help balance bacteria in the gastrointestinal tract.” (Painter, et. al., 2023).
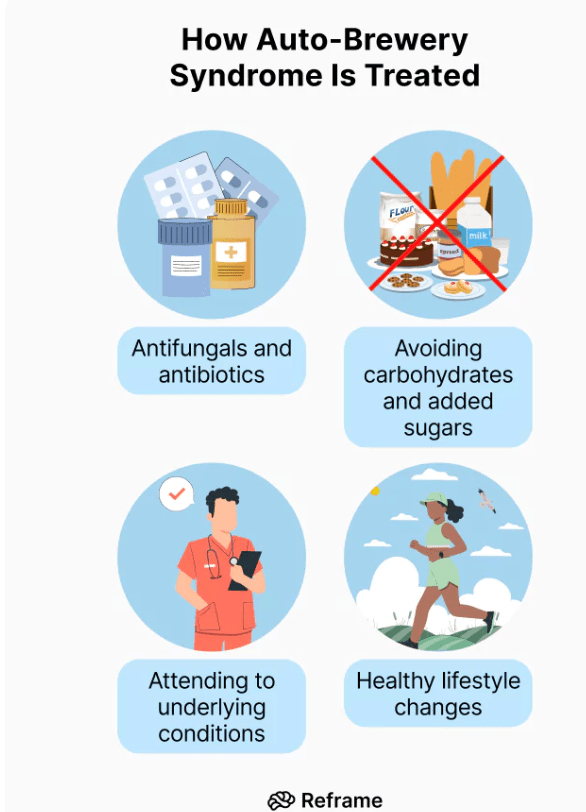
(Image from https://www.joinreframeapp.com/blog-post/what-is-auto-brewery-syndrome )
A personal story: https://www.today.com/health/disease/man-shares-auto-brewery-syndrome-symptoms-rcna77263
Malik, F.; Wickremesinghe, P.; Saverimuttu, J. (2019). Case report and literature review of auto-brewery syndrome: probably an underdiagnosed medical condition. BMJ Open Gastro 2019;6:e000325. doi:10.1136/bmjgast-2019-000325 .
Painter, K.; Cordell, B.J.; Sticco, K.I.L. (2023). Auto-Brewery Syndrome. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK513346/
