
The components of smoke from tobacco cigarettes and cannabis joints have been investigated, and many of them are known to be harmful. In fact, many of these compounds are found in both types of smoke.
In this post, we will look at the components smoke from both sources and see how they affect the health of non-smokers via the inhalation of second-hand smoke.
I. Tobacco
Please allow me to start this section with a military acronym, BLUF, i.e. “Bottom Line, Up Front”:
Smoking cigarettes is harmful to your health.
First, the deposition of tar particles deep in lung tissue induces a response which leads to a reduction in lung function:
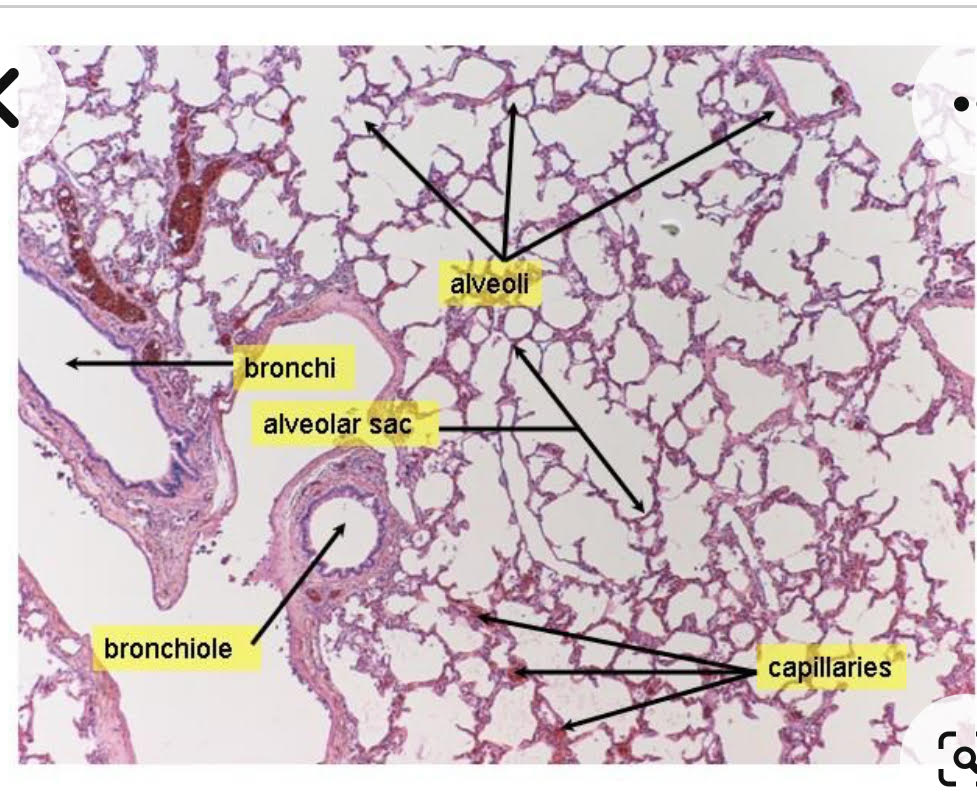
L: Photomicrograph of healthy lung; R: Photomicrograph of a lung from a smoker, showing deposition of tar particles and tissue response.
The progressive damage to the lungs will eventually become obvious when we compare the gross anatomy of lungs from a healthy lungs with lungs from a smoker:
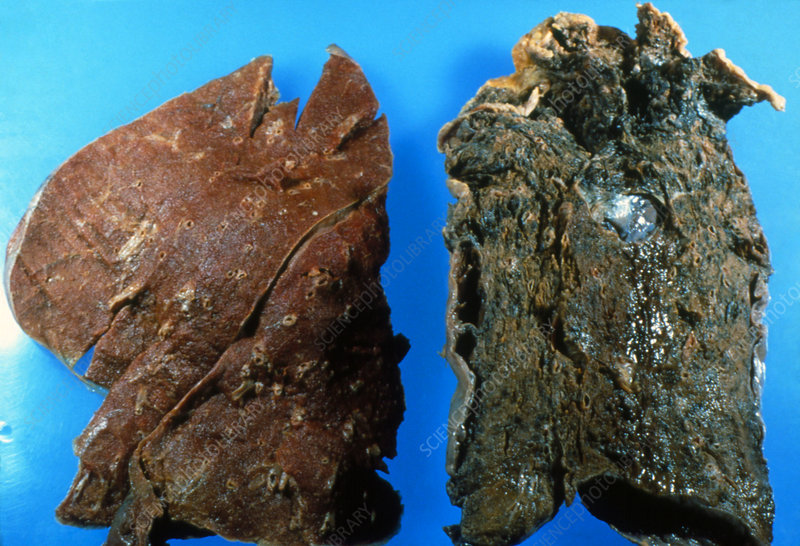
Scientists have found over 7,000 compounds in cigarette smoke, many of which are mutagenic and/or carcinogenic, of which the ones of greatest concern are the following:
These include:
- Benzene
- Tobacco-specific nitrosamines
- Benzo[α]pyrene
- 1,3-butadiene (a hazardous gas)
- Cadmium (a toxic metal)
- Formaldehyde
- Acetaldehyde
It should come as no surprise, therefore, that people exposed to secondhand smoke are exposed to the same compounds. Even though the concentrations of these compounds in the air they inhale may be lower, the harm they cause is measurable, as shown in the following image:
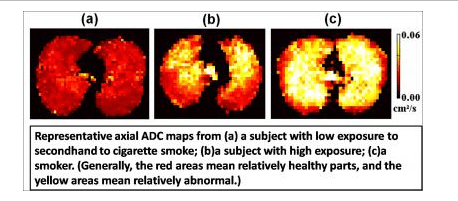
Image from https://www.eurekalert.org/multimedia/909931. Caption: The apparent diffusion coefficient (ADC) measures lung injury, indicated by different colors. Credit: The Children’s Hospital of Philadelphia and the University of Virginia; Usage Restrictions: None
The following graphic summarizes the effects of secondhand smoke on (nonsmoking) family members:
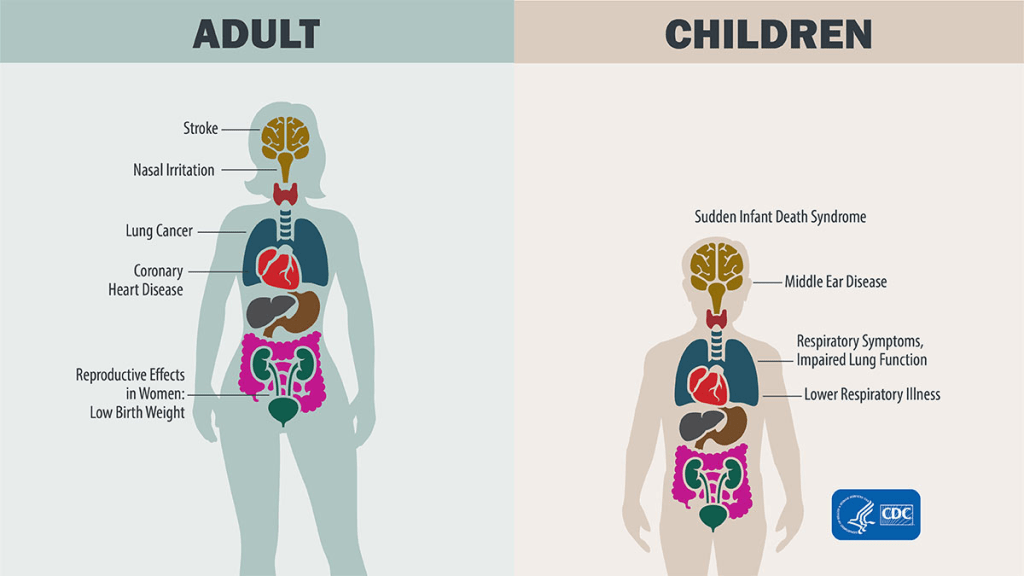
Illustration from https://www.cdc.gov/tobacco/secondhand-smoke/health.html
The following text is extracted from https://storymd.com/journal/qjo88nlhnm-secondhand-smoke/page/yvzpg5c552g-facts
Health Effects of Secondhand Smoke
There is no risk-free level of secondhand smoke exposure; even brief exposure can be harmful to health. Comprehensive smokefree policies have been successful in protecting those who do not smoke, and are the only way to fully protect their health.
Health Effects in Adults
In adults who have never smoked, secondhand smoke can cause:
- Diseases of the cardiovascular system: People who do not smoke, but are exposed to secondhand smoke at home or at work, experience a 25-30% increase in their risk of developing heart disease:
- Peripheral vascular disease, a narrowing of the leg arteries which can lead to blockage and, in some cases, amputation;
- Abdominal aortic aneurysm is a bursting of the lower part of the aorta leading from the heart;
- Increases in heart rate, cardiac index and pulse pressures: For adults who do not smoke, breathing secondhand smoke has immediate harmful effects on the heart and blood vessels. Within 5 minutes of passive smoke inhalation, increments in heart rate, cardiac index and pulse pressures can be measured (Alam, 2018);
- Secondhand smoke causes nearly 34,000 premature deaths from heart disease each year in the United States among adults who do not smoke;
- Stroke: Each year, more than 8,000 deaths from stroke can be attributed to secondhand smoke.
- Various forms of cancer:
- Lung, mouth, tongue, nose, nasal sinus, voice box, oesophagus, pancreas, stomach, liver, kidney, bladder, ureter, bowel, ovary, cervix, and bone marrow (myeloid leukaemia) Smoking related cancers accounted for nearly 21% of all cancer deaths in 2005 (Alam, 2018);
- Regarding lung cancer in particular: Lung cancer in nonsmoking individuals accounts for 15% to 20% of lung cancer cases worldwide. Furthermore, they state that in the US, the annual incidence of lung cancer in nonsmoking individuals is 14.4 to 20.8 per 100 000 person-years in females and 4.8 to 12.7 per 100 000 person-years in males. Most lung cancers in nonsmoking individuals are histologically adenocarcinomas (60%-80%) with the remainder being squamous or adenosquamous (10%-20%) and rarely small cell lung cancer (<10%) (Murphy, et. al., 2025);
- Problems with the respiratory system: In 2006, the US Centers for Disease Control and Prevention published The Health Consequences of Involuntary Exposure to Tobacco Smoke: A Report of the Surgeon General. In this book, the effects are assessed according the following criteria: Odor and Irritation; Respiratory Symptoms; Lung Function; Asthma; and Chronic Obstructive Pulmonary Disease. The conclusions in Chapter 9, Respiratory Effects in Adults from Exposure to Secondhand Smoke are quoted here:
- Odor and Irritation
- The evidence is sufficient to infer a causal relationship between secondhand smoke exposure and odor annoyance.
- The evidence is sufficient to infer a causal relationship between secondhand smoke exposure and nasal irritation.
- The evidence is suggestive but not sufficient to conclude that persons with nasal allergies or a history of respiratory illnesses are more susceptible to developing nasal irritation from second hand smoke exposure.
- Respiratory Symptoms
- The evidence is suggestive but not sufficient to infer a causal relationship between secondhand smoke exposure and acute respiratory symptoms including cough, wheeze, chest tightness, and difficulty breathing among persons with asthma.
- The evidence is suggestive but not sufficient to infer a causal relationship between secondhand smoke exposure and acute respiratory symptoms include cough, wheeze, chest tightness, and difficulty beathing among healthy persons.
- The evidence is suggestive but not sufficient to infer a causal relationship between secondhand smoke exposure and chronic respiratory symptoms
- Lung Function
- The evidence is suggestive but not sufficient to infer a causal relationship between short-term secondhand smoke exposure and an acute decline in lung function in persons with asthma.
- The evidence is inadequate to infer the presence of a causal relationship between short-term secondhand smoke exposure and an acute decline in lung function in healthy persons.
- The evidence is suggestive but not sufficient to infer a causal relationship between secondhand smoke exposure and a small decrement in lung function in the general population.
- The evidence is suggestive but not sufficient to infer a causal relationship between chronic secondhand smoke exposure and a small decrement in lung function in the general population.
- The evidence is inadequate to infer the presence or absence of a causal relationship between chronic secondhand smoke exposure and an accelerated decline in lung function.
- Asthma
- The evidence is suggestive but not sufficient to infer a causal relationship between secondhand smoke exposure and adult-onset asthma.
- The evidence is suggestive but not sufficient to infer a causal relationship between secondhand smoke exposure and a worsening of asthma control.
- Chronic Obstructive Pulmonary Disease (COPD)
- The evidence is suggestive but not sufficient to infer a causal relationship between secondhand smoke exposure and risk for chronic obstructive pulmonary disease.
- The evidence is inadequate to infer the presence or absence of a causal relationship between secondhand smoke exposure and morbidity in persons with chronic obstructive pulmonary disease.”
- Odor and Irritation
Health Effects in Infants and Children:
- Smoking during pregnancy results in more than 1,000 infant deaths annually.
- Adults exposed to secondhand smoke during pregnancy are more likely to have newborns with lower birth weight, increasing the risk of health complications.
- Infants exposed to secondhand smoke after birth have significantly higher risk of Sudden Infant Death Syndrome (SIDS).
- Chemicals in secondhand smoke appear to affect the brain in ways that interfere with its regulation of infants’ breathing.
- Infants who die from SIDS have higher concentrations of nicotine in their lungs and higher levels of cotinine than infants who die from other causes.

- Exposure to secondhand smoke causes multiple health problems in infants and young children, including:
- Ear infections
- Neural Tube Defects have been documented among babies born to women exposed to passive smoking (Alam, 2018);
- Childhood cancer (hepatoblastoma) where the father and/or mother smoked before and/or during pregnancy;
- Respiratory symptoms: (coughing, wheezing, shortness of breath):
- Acute lower respiratory infections, such as bronchitis and pneumonia: Children with asthma who encounter secondhand smoke have more severe and more frequent asthma attacks;
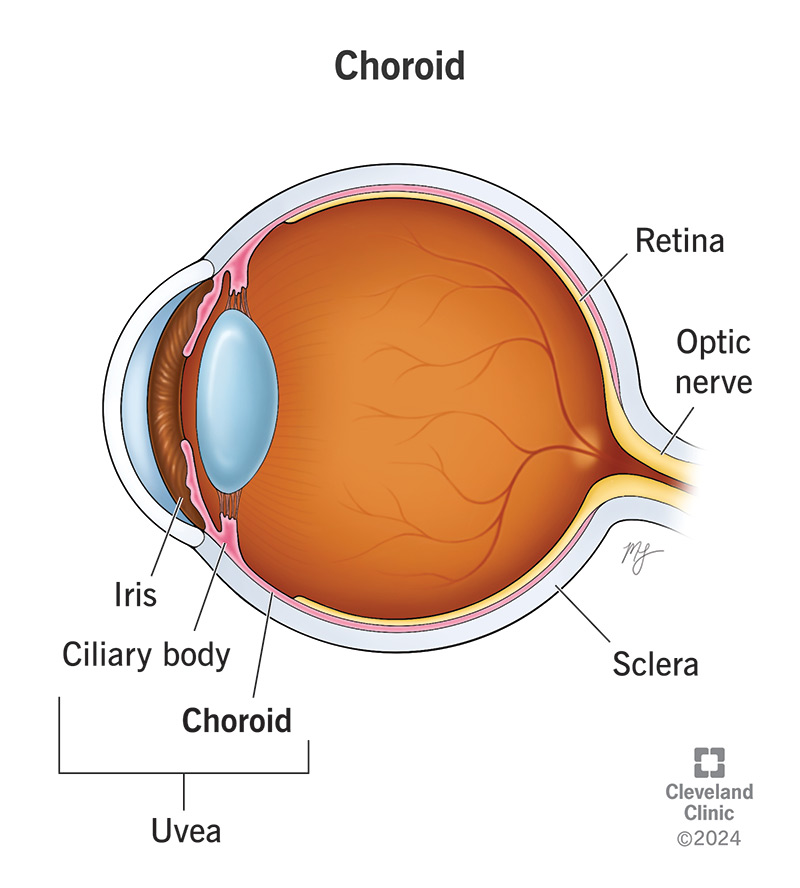
- A reduction in choroidal thickness: In a study of 1,400 children ages 6 to 8, researchers in Hong Kong found “choroidal thickness 6 to 8 micrometers thinner than those of the non-exposure group. Moreover, choroidal thickness was negatively correlated with the number of family smokers, such that for every one increase in family smoker, children’s choroids thinned by 4 to 7 micrometers, generally. So, too, for every increase of exposure to one secondhand smoker per day, choroids were reduced as much as 0.5 micrometers ( https://www.aoa.org/news/clinical-eye-care/health-and-wellness/secondhand-smoke-could-harm-childrens-eyes).”
- “The choroid is a part of the uvea, the middle layer of your eyeball’s outer wall. It’s a key supplier of blood to some of your eyes’ most critical structures. The choroid (pronounced “KOR-oid”) also plays a role in how light acts inside your eye, making it a crucial part of how you see the world around you…The choroid has two main jobs: blood supply and light absorption.” (https://my.clevelandclinic.org/health/body/choroid)
In 2016, Fernandez, et. al., reported their findings on the deleterious effects of secondhand smoke on 3,187 children (1,632 boys and 1,555 girls) aged 8-17 in Mexico City. This study was part of the Metropolitan Study to Evaluate the Chronic Effects of Pollution in School-age Children (EMPECE). They found that passive smoking, reported by half of the participants, was associated with reduced spirometric lung function and higher frequency of self-reported respiratory symptoms and respiratory infections. Levels of forced expiratory volume in 1 second (FEV1) and forced vital capacity (FVC) in individuals exposed to passive smoking were 6.8 and 14.1 ml, respectively, below those of non-exposed children. Furthermore, those values decreased with increasing number of smokers at home and with higher ozone levels. The authors point out that exposure to air pollution, including secondhand smoking, is of higher concern in children because ventilation per size is higher than in adults, an effect relevant in Mexico City, with altitude-induced hyperventilation. (Mexico City is located at an altitude of 2,240 meters.)
II. Cannabis
A. Perhaps the good news is that fewer people are being incarcerated because of possession or use of cannabis.
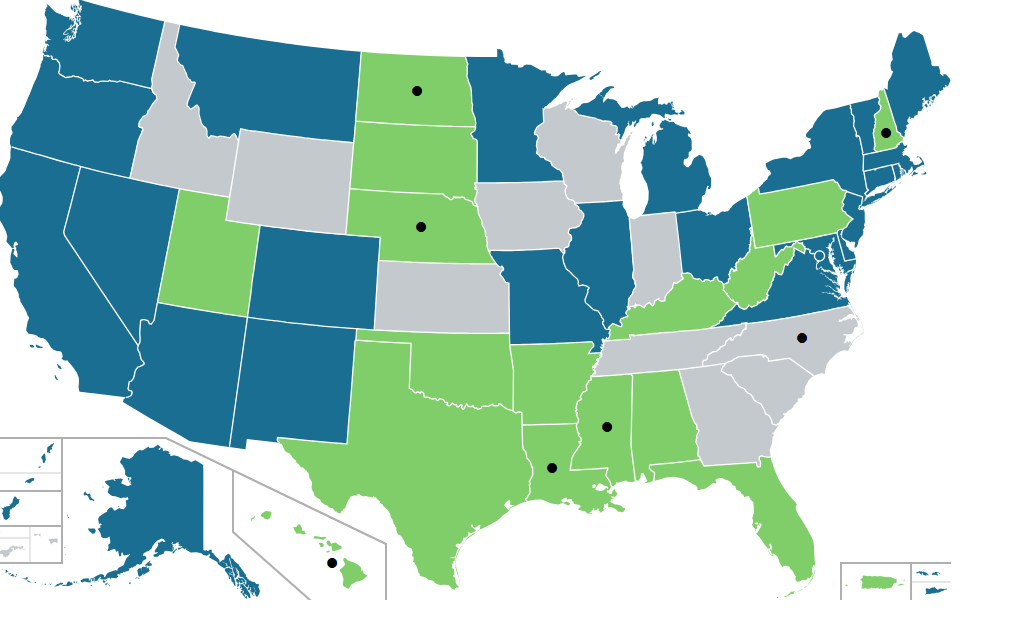
Cannabis is now legal for either medical and/or recreational use in 41 states, according to this map, downloaded from https://commons.wikimedia.org/wiki/File:Map_of_US_state_cannabis_laws.svg:

The trend towards legalization is a global phenomenon as well. The following two figures are extracted from https://en.wikipedia.org/wiki/Legality_of_cannabis :
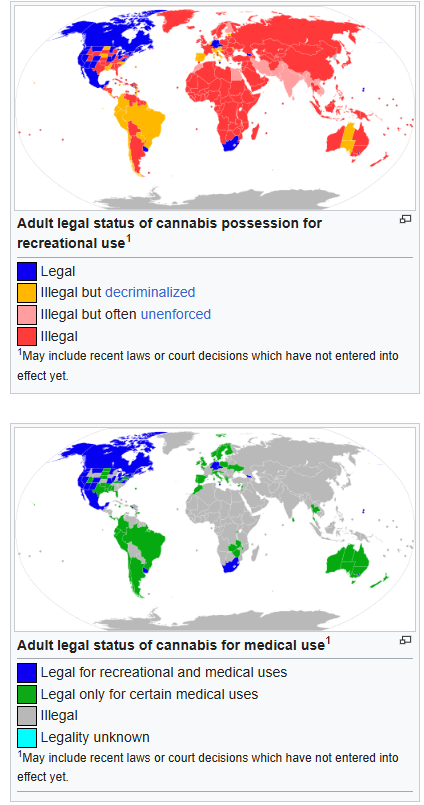
B. Proof of concept: People exposed to secondhand smoke absorb measurable amounts of THC, metabolites, and harmful chemicals.
Given the increasing number of people who are using cannabis for either medical or recreational purposes, there is a belief that, unlike tobacco smoke, marijuana smoke is benign. However, we know that it is not benign, because the smoke generated from a marijuana joint contains the same carcinogenic compounds as that generated from a tobacco cigarette (Hashibe, et. al., 2005):
- Vinyl chlorides;
- Phenols;
- Nitrosamines;
- Reactive oxygen species; and
- Various polycyclic aromatic hydrocarbons (PAHs).
- Benzene
- Acroleine
- Benzo(a)pyrene
The increased acceptance of using cannabis by the public is allowing scientists to study the effects of secondhand smoke.
In 2015, a group of scientists published a series of 3 articles to determine the effects of secondhand smoke. The protocol for these studies was similar:
One group of experienced cannabis smokers were recruited to smoke cannabis and to produce a cloud of smoke in both ventilated and unventilated conditions. A second group of non-smoking individuals were recruited to measure the concentration of THC and metabolites in their blood and urine, and to measure possible sedative drug effects and performance on the Digit Symbol Substation Task (DSST).
Copyright laws prevent me from copying and pasting the photo of smoke in the unventilated room setting, but you REALLY need to look at Figure 2 of Cone, et. al, 2015a, which you can access at https://pmc.ncbi.nlm.nih.gov/articles/PMC4342697/pdf/bku116.pdf.

(Image generated by AI.)
These studies established that those individuals exposed to secondhand smoke showed the following:
- Measurable amounts of THC and metabolites could be detected in the urine and blood;
- Minor increases in heart rate;
- Mild to moderate self-reported sedative drug effects; and
- Impaired performance on the Digit Symbol Substitution Task (DSST) (Cone, et. al., 2015a; Herrmann, et. al., 2015; Cone, et. al., 2015b)
Perhaps one could say that this series of article established proof of concept of the obvious, that people exposed to secondhand smoke will incorporate the active drug, its metabolite(s), and any other compounds earlier.
The transfer of THC or its metabolites to family members does not require a special chamber where the cannabis smoke becomes so dense that it obscures vision. The purpose of a more recent study (Tripathi, et. al., 2025) was to test the association of in-home cannabis smoking with the detection of urinary cannabinoids in children living at home.
The final analytic sample in this study consisted of 275 households. After enrollment, staff members installed instruments in the houses to monitor fine air particles and air nicotine dosimeters. Enrolled parents or guardians were assessed activities which would generate air particles in the previous 7 days.
Each parent was provided with a urine collection kit, with instructions regarding how to collect urine samples from the enrolled child. In-home cannabis smoking was measured using data from air particle monitoring and reported in-home smoking in the past 7 days, concurrent with the air particle monitor data collection. Urine samples from children were examined for the presence of THC and two metabolites, OH-THC and COOH-THC.
Their results showed the following:
- A total of 275 children were analyzed;
- The average age of these children was 3.6;
- Participating households had a mean 2.9 daily smoking events;
- Parents of 29 households (10.6%) reported that cannabis was smoked inside their home in the past 7 days, and a total of 75 children (27.3%) had detectable cannabis exposure biomarkers in their urine;
- Not surprisingly, the odds of detecting cannabis biomarkers in children’s urine among households that reported in-home cannabis smoking in the past 7 days were 5.02 times the odds of households without reported in-home cannabis smoking.
The fact that over 25% of children had detectable amounts of cannabinoids in their urine has implications regarding public health measures that safeguard children’s health, especially at a time when the consumption of cannabis is increasing.
C. Evidence that secondhand smoke causes harm
1. Animal studies
Wang, et. al. (2015) describe subtle changes in vascular health that occur among rats exposed to secondhand cannabis smoke. In their study, female Sprague-Dawley rats were exposed to cannabis smoke in order to measure changes in arterial flow-mediated dilation (FMD), the extent to which their arteries would vasodilate in response to increased blood flow. One minute of exposure impaired FMD to a comparable extend as impairment from equal concentrations of tobacco secondhand smoke, but recovery was slower. In fact, FMD remained impaired for at least 90 minutes.
The implication of this finding is significant. FMD ensures sufficient blood flow to peripheral tissues and the heart. They state “Decline in FMD precedes the development of atherosclerosis and is likely important in its pathogenesis.” It is interesting to note, however, that FMD is impaired by 1 or more constituents of smoke NOT specific to either cannabis OR tobacco.
2. Effects on children
Moore, et. al. (2023) describes a study conducted on 81 mother-child pairs recruited between 2010 and 2014 from outpatient obstetrics clinics at the University of Colorado Hospital. Seven common common cannabinoids (THC, CBD and their metabolites) were measured in maternal urine collected mid-gestation and child urine collected when the child reached 5 years of age.
In this study, 7% (n=6) of the children had prenatal exposure to cannabis, while 12% (n=10) had postnatal exposure to cannabis. They found THC to be the most common cannabinoid detected in pregnancy, while CBD was the most cannabinoid detected in childhood. “Postnatal exposure to cannabis was associated with more aggressive behavior and oppositional/defiant behaviors, and weaker receptive language. By contrast, prenatal exposure to cannabis was associated with fewer internalizing behaviors and fewer somatic complaints.”
They conclude that postnatal exposure to cannabis brings greater risk for behavioral and cognitive problems among 5-year-olds, independent of prenatal and postnatal exposure to alcohol.
III. The problem may not be the native chemicals in tobacco or in cannabis, but rather the tar and carcinogenic compounds generated by the pyrolysis of the leaves.
The pyrolysis of either tobacco or cannabis leaves generates fine particles, carcinogens which adhere to those particles, and toxic gases, such as carbon monoxide and ammonia.

Image of Main Stream Second-hand Smoke (source: blog.whitecloudelectroniccigarettes .com). B. Side Stream Smoke. Side stream smoke is that part of smoke which automatically goes off from a burning cigarette or Cigars and other burning forms of tobacco. Side stream smoke contributes about 85 percent of second-hand smoke. Volatile Organic Carbon (VOC) and Particulate Matter (PM) emissions in total, Side Steam (SS)and Main Stream (MS) smoke were measured (Charles, Simone, M et al, 2007) for three types of research cigarettes obtained from the Kentucky Tobacco Research and Development Centre (Lexington, KY).
P.S.:
Alam, S.M. (2018). Second-hand Tobacco Smoke (ETS) – Findings of an Australian Case Study and How Dhaka can read the Benefit from the Research Outcome. International Journal of Social Sciences and Humanities Invention 5(09):4959-4968. DOI: 10.18535/ijsshi/v5i9.01.
Centers for Disease Control and Prevention(US): 2006. The Health Consequences of Involuntary Exposure to Tobacco Smoke: A Report of the Surgeon General.
Cone, E.J.; Bigelow, G.F.; Herrmann, E.S.; Mitchell, M.M.; LoDico, C.; Flegel, R.; Vandrey, R. (2015a). Non-Smoker Exposure to Secondhand Cannabis Smoke. I. Urine Screening and Confirmation Results. Journal of Analytical Toxicology 39:1-12. doi:10.1093/jat/bku116 .
Cone, E.J.; Bigelow, G.F.; Herrmann, E.S.; Mitchell, MJ.M.; LeDico, C.; Flegel, R.; Vandrey, R. (2015b).Non-Smoker Exposure to Secondhand Cannabis Smoke. Journal of Analytical Toxicology 39:497-509. doi:10.10.1093/jat/bks070.
Fernandez-Plata, R.; Rojas-Martinez, R.; Martinez-Briseno, D.; Garcia-Sancho, C.; Perez-Padilla, R. (2016). Effect of Passive Smoking on the Growth of Pulmonary Function and Respiratory Symptoms in Schoolchildren. Revista de Investigacion Clinica 68:119-127.
Hashibe, M.; Straif, K.; Tashkin, D.P.; Morgenstern, H.; Greenland, S.; Zhang, Z-F. (2005). Epidemiologic review of marijuana use and cancer risk. Alcohol 35(3):265-275.
Herrmann, E.S.; Cone, E.J.; Mitchell, J.M.; Bigelow, G.E.; LoDico, C.; Flegel, R.; Vandrey, R. (2015). Non-Smoker Exposure to Secondhand Cannabis Smoke. II. Effect of Room Ventilation on the Physiological, Subjective and Behavioral/Cognitive Effects. Drug Alcohol Depend. June 1:151:194-202. doi:10.1016.drugalcdep.2015.03.019.
Moore, B.J.; Salmons, K.A.; Hot, A.T.; Swenson, K.S.; Bates, E.A.; Sauder, K.A.; Shapiro, A.L.B.; Wilkening, G.; Kinney, G.L.; Neophytou, A.M.; Sempio, C.; Klawitter, J.; Christians, U.; Dabelea. (2023). Associates between Prenatal and Postnatal Exposure to Cannabis with Cognition and Behavior At Age 5 Years: The Health Start Study. International Journal of Environmental Research and Public Health. 20, 4880. https://doi.org/10.3390/ijerph20064880.
Murphy, C.; Pandya, T.; Swanton, C.M.D.; Solomon, B.J. (2025). Lung Cancer in Nonsmoking Individuals: A Review. JAMA, Published Online: October 20, 2025. doi:10.1001/jama.2025.17695 .
Wang, X.; Derkahshandeh, R.; Liu, J.; Narayan, S.; Nabavizadeh, P.; Le, S.; Danforth, O.M.; Pinnameneni, K.; Rodriguez, A.S.; Luu, E.; Siervers, R.E.; Schick, S.F.; Glantz, S.A.; Springer, M.L. (2016). One Minute of Marijuana Secondhand Smoke Exposure Substantially Impairs Vascular Endothelial Function. J. Am Heart Assoc. 5:e003858. doi: 10.1161/JAHA.116.003858.

